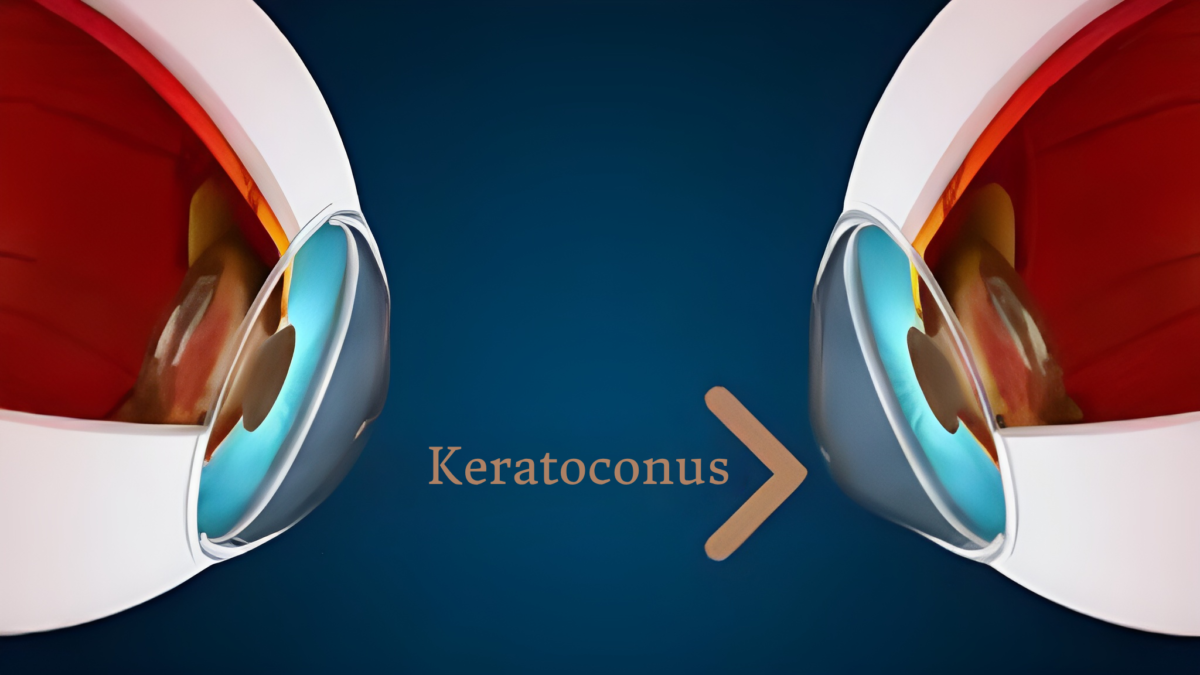
WHAT IS KERATOCONUS?
Keratoconus is a progressive condition in which the cornea thins, developing a cone-like bulge. The condition impacts the structure of the cornea, which is unable to maintain the natural round shape of the eye, leading to vision deterioration. In the initial stages, this condition may be treated with glasses or contact lenses, but as eyesight continues to deteriorate over time, treatment with Intacs implantation may be the optimal solution.

WHAT ARE INTACS FOR KERATOCONUS?
Intacs are tiny, clear arcs of specialized plastic. They are inserted into the inner structure of the cornea to provide strength and stability. When inserted into the eye, the device flattens the cornea to restore the natural dome shape. This procedure can help correct vision but often still requires the client to wear glasses or contacts. Some clients who were previously unable to wear contacts due to the discomfort associated with the misshapen cornea can now wear them comfortably, as the bulge is flattened.
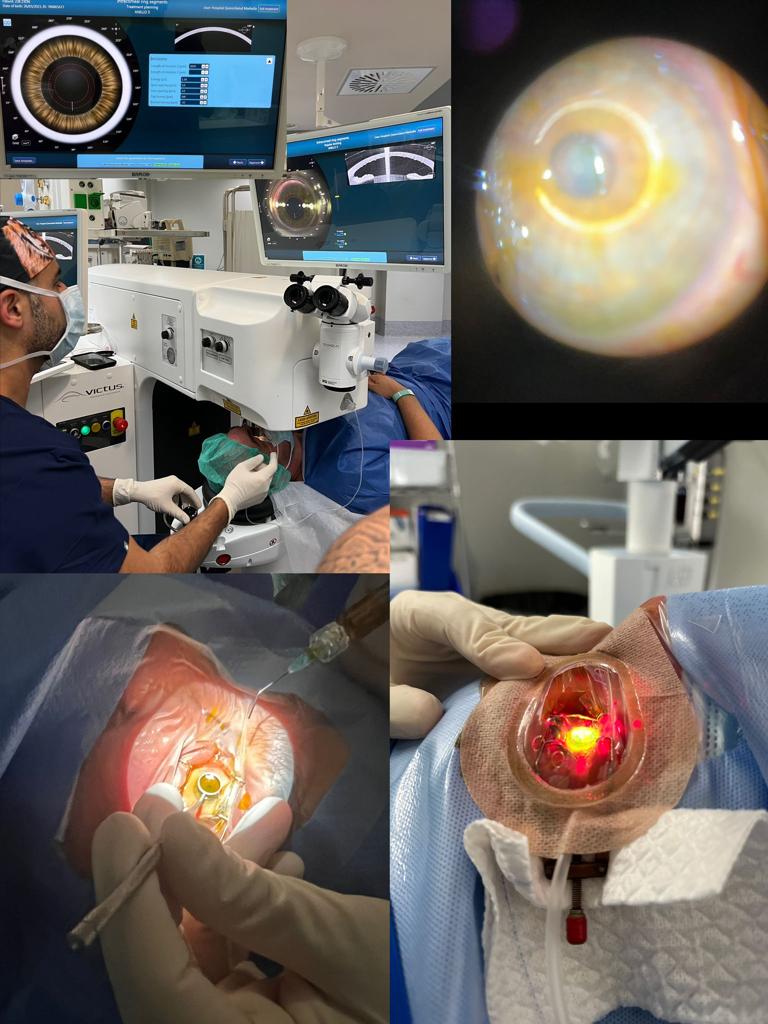
SLOWING KERATOCONUS PROGRESSION
This treatment has a very crucial added benefit. It works to slow the progression of keratoconus. Residual vision issues can be addressed with
PRK. Implanting this groundbreaking medical device can help avoid significant visual impairment, blurred vision, and other symptoms such as light sensitivity.
The procedure involves several steps:
- The eye is numbed with topical anesthetic drops.
- The eye will be held open with a special device to halt blinking, but this is not uncomfortable.
- A tiny incision is created with our advanced laser system.
- The layers of the cornea are gently and
delicately separated, and the Intacs device. is placed in the ideal location to flatten the bulge in the cornea.
PROTECTING YOUR EYES FROM KERATOCONUS
The micro-thin, semi-circular Intacs rings are delicately and precisely inserted into the cornea, flattening the cone-shaped protrusion and altering the shape and location of the bulge. These tiny rings both remodel the shape of the cornea and reinforce it, treating contour irregularities to improve eyesight. Depending on the extent of the condition, you may still need to use glasses or contacts, but the eyes are now reinforced and protected from the more
serious stages of keratoconus.
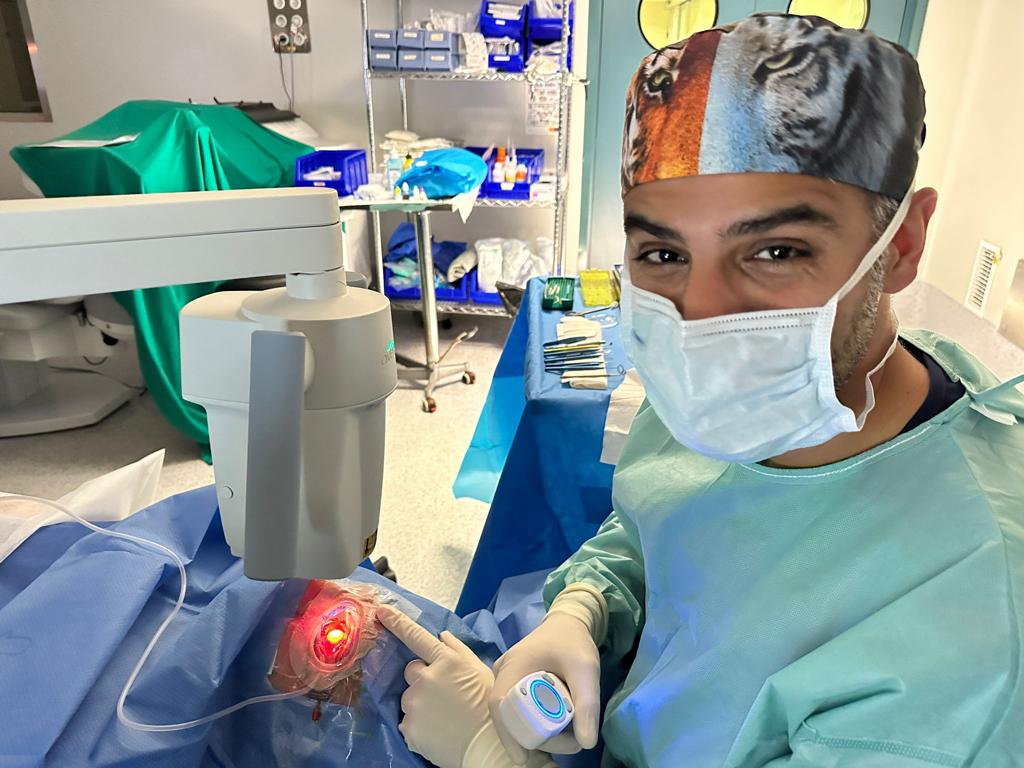
World-class vision correction treatments
If you have been diagnosed with keratoconus, you are likely feeling anxious and concerned about losing your vision. Dr. Ali Nowrouzi and the professional team 100% committed to providing state-of-the-art solutions for keratoconus.
Dr. Nowrouzi 's credentials, experience, track record, and inventions have led to his reputation as one of the best eye surgeons in the world, and he caters to clients locally and from around the globe.
Keratoconus is an ectatic corneal disease characterized by a progressive structural deformation and thinning of the cornea affecting up to 1:375 in some special populations. The most commonly studied techniques for the treatment of keratoconus are intrastromal corneal ring segment (ICRS) and collagen crosslinking (CXL). However, Dr. Nowrouzi who is a specialist in corneal disease and pathologies with years of experience in the treatment of this corneal pathology and as an active member of international society of keratoconus tries to help his patients with the modern and last generation of advanced techniques, like wavefront and topographic guide photorefractive keratectomy (ttPRK) with or without CXL and Phakic intraocular lens (pIOL) implantation.
Combined approaches like ICRS or PRK- crosslinking (CXL) protocols aim to regularize the cornea, but such treatments do not target the patient's refraction issues, especially in the presence of high anisometropia. Because of this, phakic intraocular lenses (pIOL) play a critical role in the visual rehabilitation of keratoconus patients, usually suffering from high refractive errors with significant levels of anisometropia, limiting the use of spectacles.
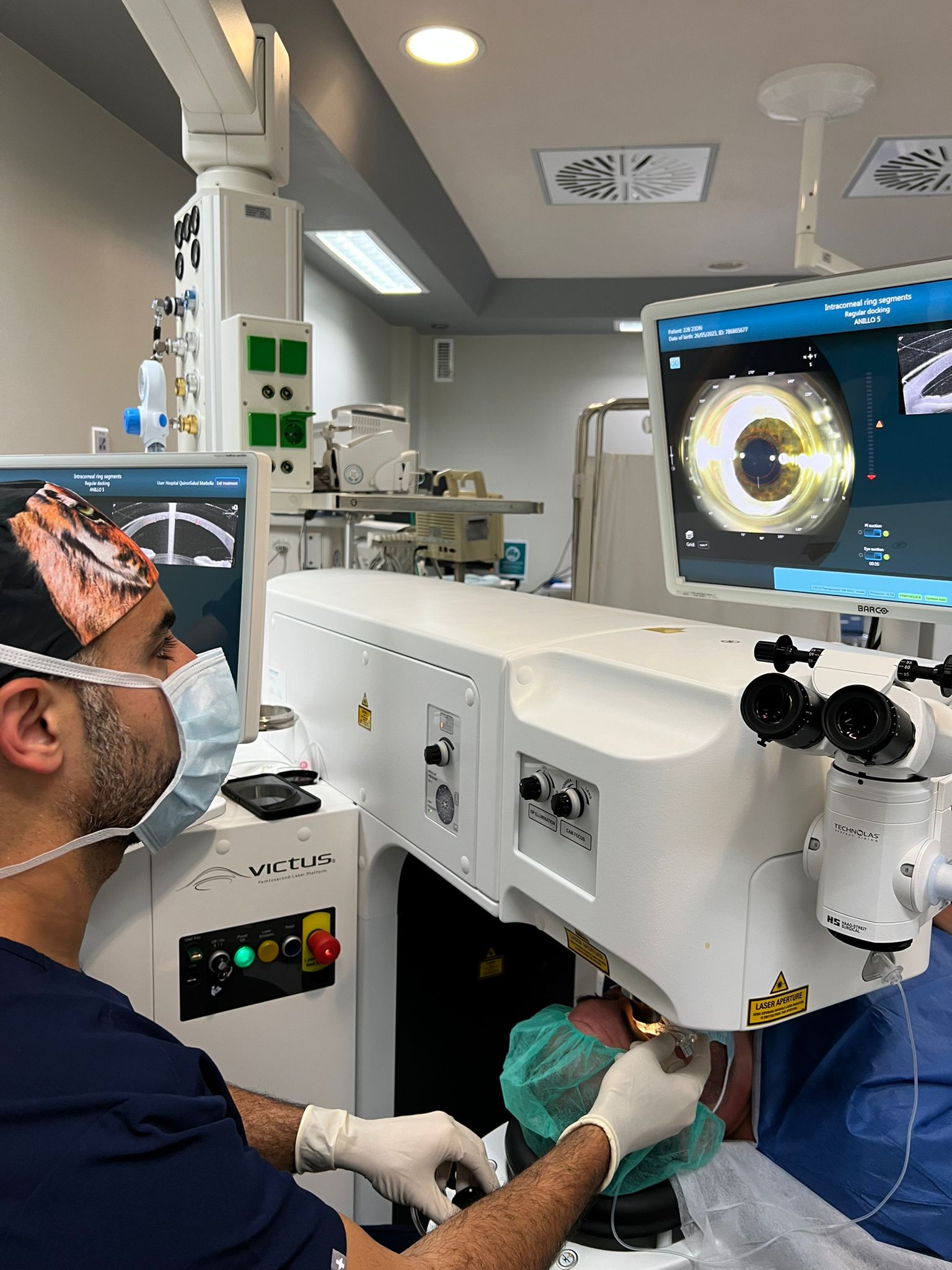
Keratoconus: Understanding and Managing a Complex Corneal Condition
Introduction:
Keratoconus is a progressive corneal disorder characterized by the thinning and bulging of the cornea, leading to visual distortion and impairment. This essay aims to provide a comprehensive overview of keratoconus, including its causes, symptoms, diagnosis, and management options. By understanding this complex condition, individuals can make informed decisions regarding their treatment and maintain optimal eye health.
Overview of Keratoconus:
Keratoconus affects the structure of the cornea, which is responsible for focusing light onto the retina. In this condition, the cornea gradually thins and assumes a conical shape, resulting in irregular astigmatism and blurred vision. The exact cause of keratoconus is still not fully understood, but it is believed to be influenced by genetic and environmental factors.
Symptoms and Diagnosis:
The symptoms of keratoconus often manifest during the teenage years or early adulthood. Common signs include progressive nearsightedness or astigmatism, distorted and ghosting vision, increased sensitivity to light, and frequent changes in eyeglass prescriptions. Proper diagnosis is crucial for timely intervention. Ophthalmologists employ various diagnostic tools such as corneal topography, corneal pachymetry, and slit-lamp examination to evaluate the shape, thickness, and integrity of the cornea.
Management Options:
1. Spectacles and Contact Lenses: In the early stages of keratoconus, eyeglasses or soft contact lenses may help correct the refractive error and improve visual acuity. However, as the condition progresses, rigid gas permeable (RGP) or scleral lenses may be required to provide better corneal support and visual clarity.
2. Corneal Collagen Cross-Linking (CXL): CXL is a minimally invasive procedure that aims to halt the progression of keratoconus. It involves the application of riboflavin (vitamin B2) eye drops followed by exposure to ultraviolet A (UVA) light. This combination strengthens the cornea by promoting the formation of cross-links within its collagen fibers, preventing further thinning and bulging.
3. Intrastromal Corneal Ring Segments (ICRS): ICRS, commonly known as corneal implants or intacs, are tiny plastic rings inserted into the cornea to flatten its shape and improve visual acuity. These implants redistribute the corneal tissue, enhancing its structural stability and reducing astigmatism.
4. Partial and Full-Thickness Corneal Transplants: In severe cases of keratoconus where vision cannot be adequately corrected by other means, corneal transplantation may be considered. Depending on the extent of corneal involvement, options include deep anterior lamellar keratoplasty (DALK) or penetrating keratoplasty (PK), where the affected cornea is replaced with a healthy donor cornea.
5. Advancements in Treatment: Recent advancements in keratoconus management include techniques such as Descemet's membrane endothelial keratoplasty (DMEK) and Descemet's stripping automated endothelial keratoplasty (DSAEK), which focus on replacing only the innermost layer of the cornea, providing faster recovery and better visual outcomes.
Lifestyle Modifications and Support:
Living with keratoconus requires proactive management and lifestyle adjustments. Protecting the eyes from excessive ultraviolet (UV) exposure by wearing sunglasses, practicing good eye hygiene, avoiding eye-rubbing, and attending regular eye examinations are essential. Support groups and online communities provide a valuable platform for individuals to share experiences, seek advice, and find emotional support from others facing similar challenges.
Conclusion:
Keratocon
us is a complex corneal condition that requires a multidisciplinary approach for its management. Through early diagnosis and appropriate treatment, individuals with keratoconus can minimize visual impairment and maintain a good quality of life. Ongoing research and advancements in treatment options offer hope for improved outcomes, emphasizing the importance of regular eye examinations and seeking specialized care from ophthalmologists experienced in managing keratoconus. By understanding this condition and exploring available management options, individuals can take control of their eye health and enjoy optimal visual function.