Corneal lamellar transplants
Dr. Nowrouzi is the specialist of all type of new generation of lamellar corneal transplants such as Deep Anterior Lamellar keratoplasty (DALK), Descemet's membrane endothelial keratoplasty (DMEK),
and Descemet's stripping automated endothelial keratoplasty (DSAEK).
Descemet's membrane endothelial keratoplasty (DMEK) is a partial thickness cornea transplant where the host Descemet membrane (DM) and endothelium are replaced by donor DM and endothelium.
This is different than Descemet's stripping automated endothelial keratoplasty (DSAEK) where donor DM, endothelium, and posterior stroma replace host DM and endothelium. DMEK and DSAEK are both endothelial keratoplasty procedures, in contrast to a full thickness penetrating keratoplasty_(PK).
Endothelial keratoplasty procedures are not suitable for patients with healthy corneal endothelium, such as patients with stromal scarring or keratoconus. These patients still require DALK or PK.
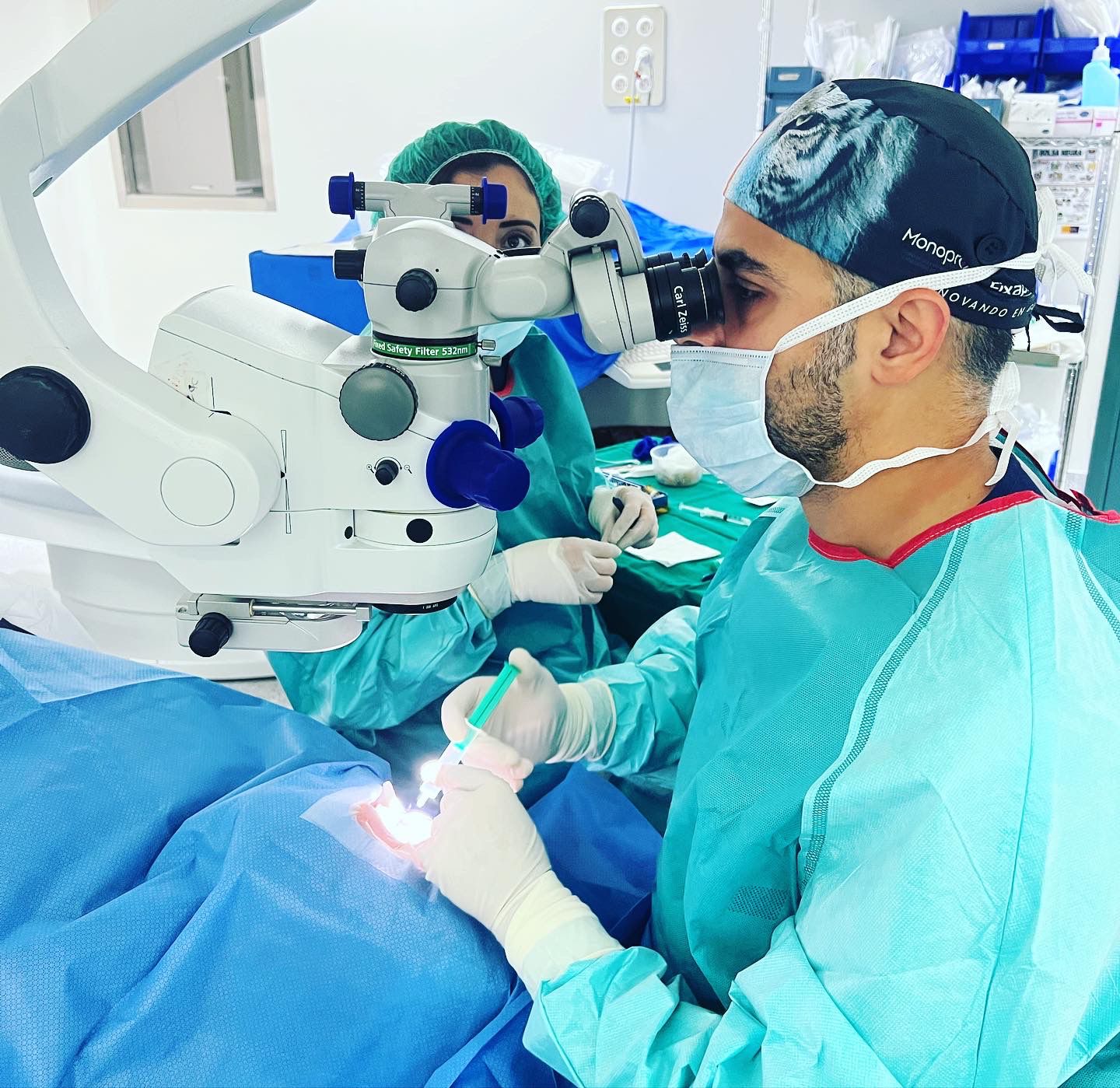
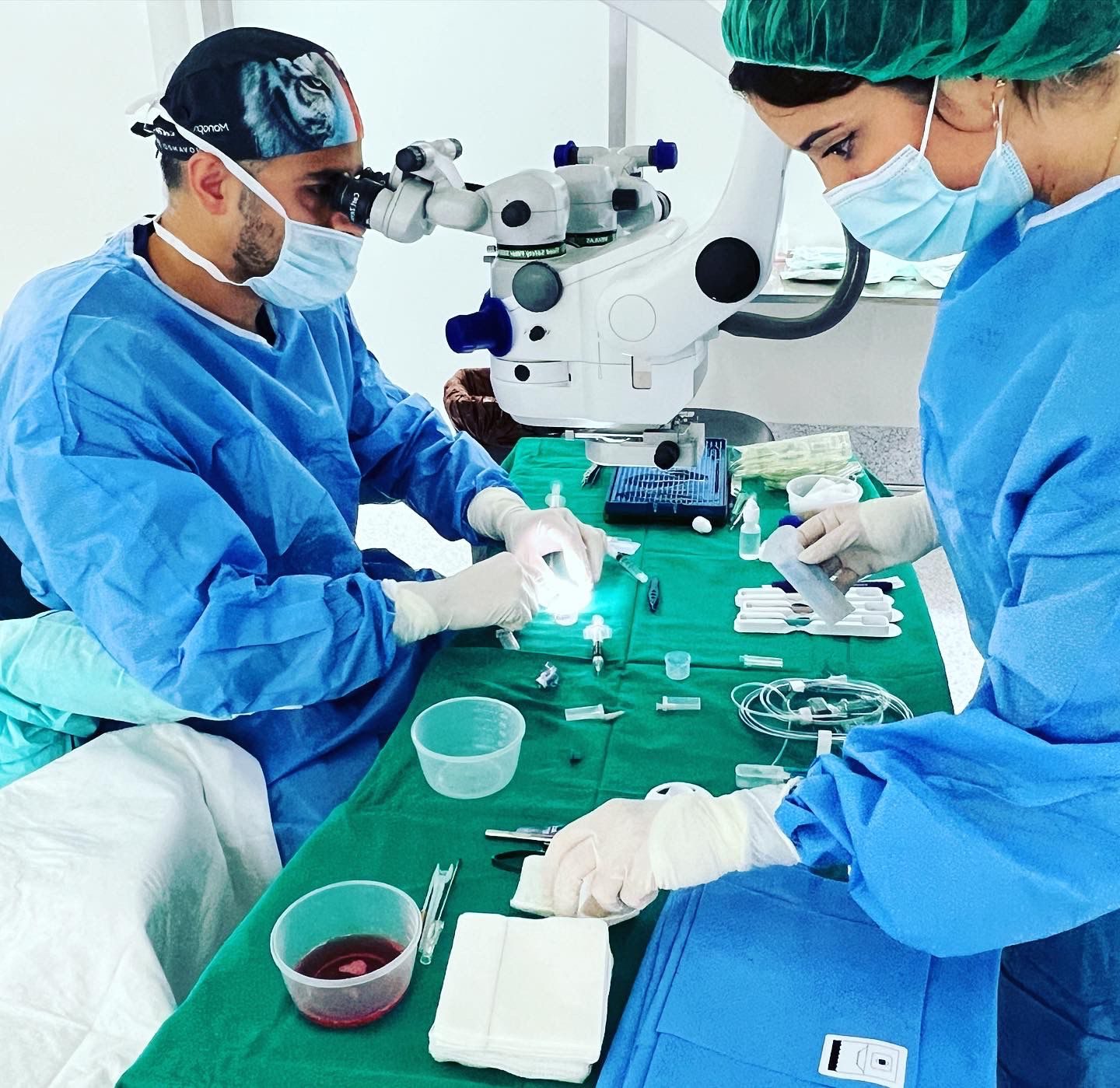
Good candidates for DMEK
- Fuchs' endothelial dystrophy
- Posterior polymorphous membrane dystrophy
- Congenital hereditary endothelial dystrophy
- Bullous Keratopathy
- Iridocorneal endothelial (ICE) syndrome
- Failed endothelial keratoplasty
Not suitable or highly complex scenarios for DMEK
-
- Stromal scarring
- Keratoconus
- Inability to lie flat
- Hypotony
- Aphakia
- Aniridia or large iris defects
- Anterior chamber intraocular lens
- Previous glaucoma surgery
- Risk of tissue loss through tubes, trabeculectomies, or peripheral iridectomies
- Postoperative gas bubble loss with resulting graft detachment can occur
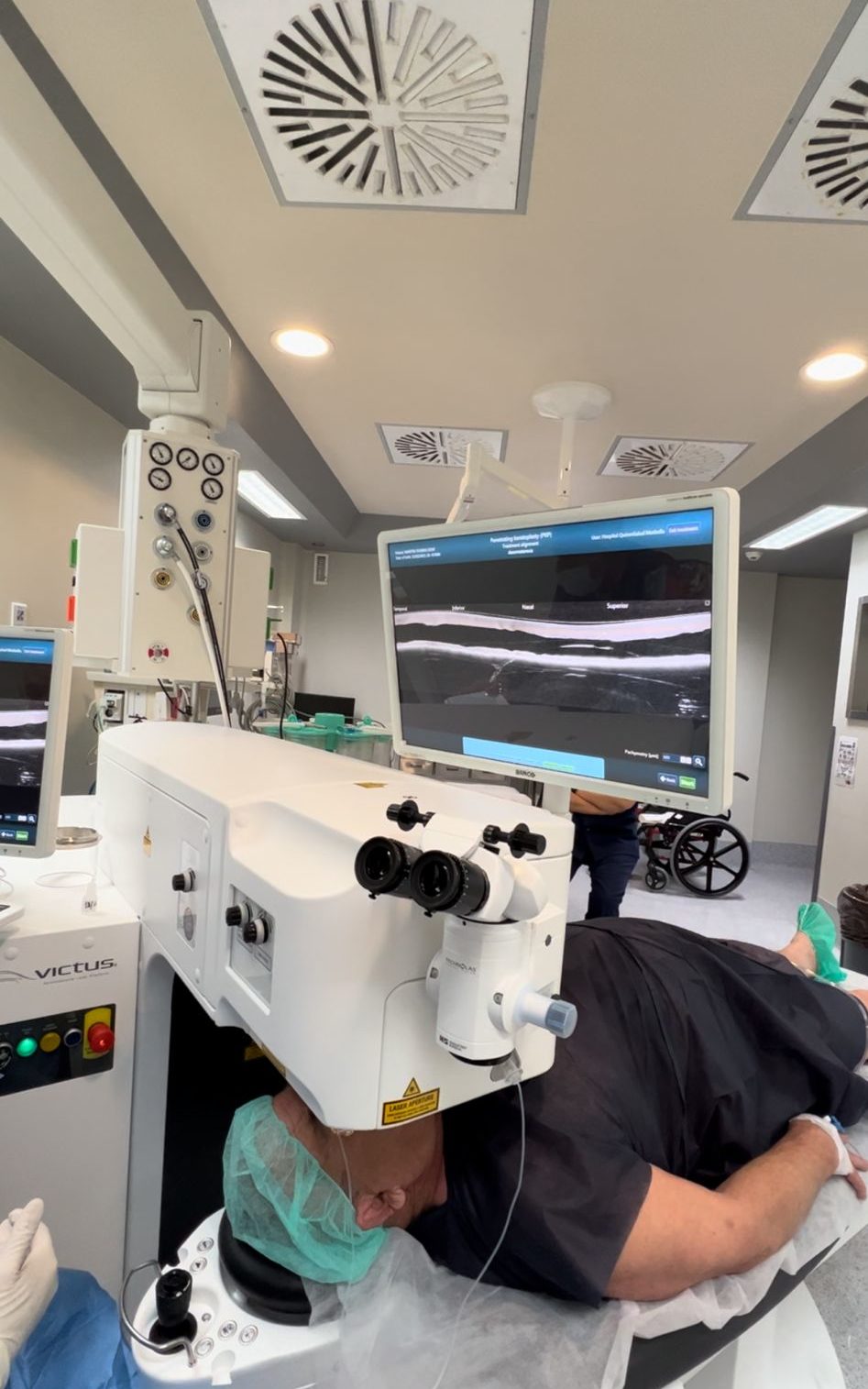
DMEK is a relatively new procedure and surgeons continue to develop many new exciting techniques and strategies.Dr. Nowrouzi by means of new technologies such as the use of real-time intraoperative OCT and femtosecond laser with DMEK offers these new generation technologies to his patients.. Eye banks will likely continue to play an important role in DMEK surgery, and their involvement with pre- stripping DMEK tissue decreases tissue wasting by the surgeon during preparation. Enhancing endothelial cell number and viability should remain an important research focus. Descemet membrane endothelial transfer gene therapy, or Rho-associated kinase inhibitors are particularly exciting areas that Dr. Nowrouzi for the first time started these new treatments in the region and offers all these new generation therapeutic approaches to his patients.
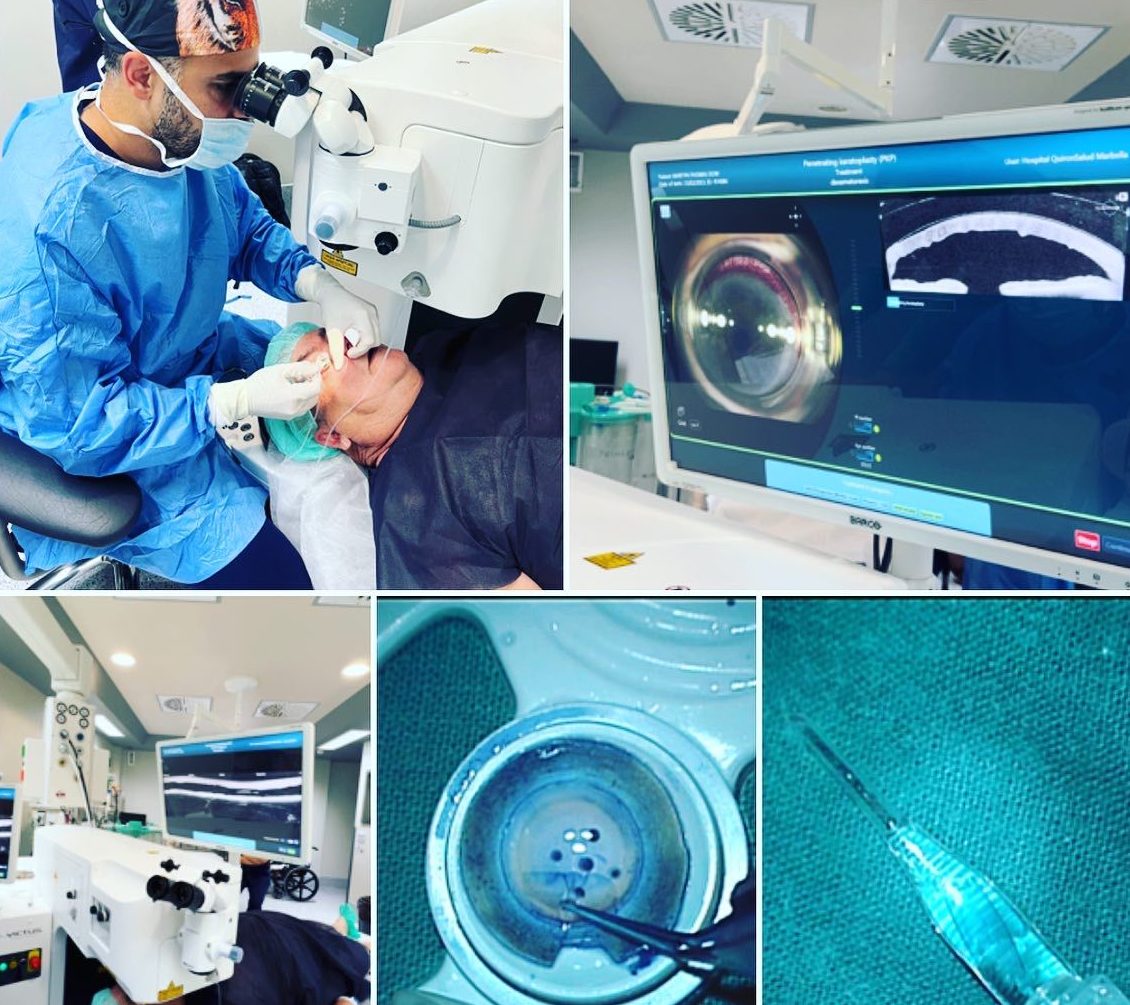
Advantages of DMEK over DSAEK
DMEK has been shown to have superior visual outcomes when compared to DSAEK. In multiple studies where patients had DSAEK in one eye and DMEK in the fellow eye, significantly better visual acuity and preference were reported in the DMEK eye. Guerra et al. reported a best corrected visual acuity in a DMEK group at 1 year of 20/24 compared to 20/32 in a DSAEK group. 85% reported a better quality of vision in the DMEK eye. Endothelial cell loss at 1 year was 31% in DMEK eyes and 34% in DSAEK eyes.
However, some studies suggest that DSAEK visual outcomes can be improved by ultra-thin tissue. Though recovery is slower with ultra-thin DMEK versus DMEK, final visual outcomes at 1 year are comparable. If the ultra-thin DSEK technique continues to improve, the ease and reliability of it may decrease the utilization of DMEK.
DMEK also has a lower immunologic rejection rate and has the advantage of using a smaller incision (2.8 mm) than DSAEK (5 mm).